A QUESTION OF HEALTH – REDUCING RE-OFFENDING
BY LOUISE GALLAGHER, Human / Health Improvement Lead (Community Justice),
NHS Greater Glasgow & Clyde
What has health got to do with reducing re-offending? As a professional working in Health Improvement this is a question I am often asked. Writing this article has given me the opportunity to reflect on that question.
I have worked in Health Improvement in the Community Justice field for a number of years now and looking back I can see why this question is asked – surely reducing re-offending is about detecting crime and punishing the people who commit those crimes? It is a question I might have asked myself in times gone by. However, with the benefit of better understanding, that question is now much easier to answer by asking different questions – what came before the offending behaviour – what brought people to the place in their lives where they are committing crime?
Too many of the people who come into the justice system have often severe mental health problems and addiction issues, to a substantially higher prevalence than the general population. They also experience multiple barriers to accessing the services they need. Although it is complex, broadly speaking we can regard crime as a symptom of wider social inequality (including health inequality) and deprivation. Contributed to by many organisations and agencies and Published by Health Scotland in 2017, ‘Reducing Offending, Reducing Inequalities – Achieving ‘Better Health, ‘Better Lives’ Through Community Justice’, provides a good explanation of this and the supporting data. The paper defines Health Inequality as the ‘unfair difference in people’s health across social groups and between different population groups’ – including those in the Criminal Justice System.
Trauma and Adverse Childhood Experiences are inextricably linked to this argument around inequality and deprivation, I won’t go into this in any detail as I am reliably informed that separate articles in this Annual Report cover these topics, see for example Severe and Multiple Disadvantage – At the Root of Offending Behaviour and Meeting the Challenge from the Roots Up – At the Centre of Community Justice are People who Need Support.
We, as health professionals, understand that much earlier societal intervention is needed to stem the flow of people coming into the justice system. However, from a Community Justice perspective, this would be from the earliest point that people come into contact with the Justice System, be that as a young person deemed at risk of offending behaviour, those that have been arrested, to supporting those in prison and those being liberated back to their community after serving a community or prison sentence.
At every touch point of the system, is an opportunity we have to support people’s health needs, and in so doing, is an opportunity to give people the tools they need to set themselves on a different pathway; away from crime and the harm that causes not only to themselves, but to individual communities and society as a whole.
The rest of this article tells the story of just some of the interventions and initiatives that Health lead on as partners in Community Justice Glasgow – playing our part to reduce some of the harm that Social Inequality has resulted in and to reduce the risk of further offending to the benefit of everyone on Glasgow.
Community Justice Health Needs Assessment – In the Article ‘A Place for Health Improvement – Skilling Up & Supporting Community Payback Staff’ (2018-19 Annual Report), I had reported on our plans to commission a comprehensive Health Needs Survey of those in the Criminal Justice System (the first of its kind in Scotland!). I am pleased to report that the Commissioning Brief and agreement to proceed has been reached with partners. A Steering Group was established with commissioning due to take place March 2020. Unfortunately progress stalled as a result of CoVid19. Recovery planning is underway and we hope to have a contractor in place and the survey under way over 2020/2021, and to be able to report the findings next year – WATCH THIS SPACE!.
NHSGG&C Employability and Recruitment Project – A Widening Access Partnership Group was established, with its first meeting taking place in Jan 2020. Membership of the group has been expanded to include, amongst others, Department for Work and Pensions (DWP), Skills Development Scotland (SDS) and Local Employability Leads. A brief dissemination paper, detailing the purpose and aim of the Partnership has been agreed with the group.
The NHS Strategic Group (primarily involving NHS HR) was due to meet March 2020, however, this was stalled due to COVid19. Progress will be reinstated 2020/21 to finalise details of the work programme of Recruitment Staff Training, Recruiting Manager Training and connecting with development/expansion and work with Partnership group. Further Meetings of Partnership and Strategic Group will be scheduled.
Community Payback Orders – Other Health Activity
The Scottish Government’s Mental Health Strategy 2017 – 2027 takes an early intervention and preventative approach to mental health and well-being, and the commitment to provide universal training on mental health and mental health first aid.
Developing on the success of training to staff on Scotland’s Mental Health First Aid in 2018/19, in partnership with Glasgow Health and Social Care Partnership, Justice Colleagues and Unpaid Work Service Providers, have established a Health Improvement Planning group. In 2019/2020, the Group, informed by the National Mental Health Improvement & Suicide Prevention Framework (NHS Education for Scotland, 2019), has successfully planned and delivered sessions on Mental Health Awareness (commissioned from Glasgow Association for Mental health GAMH), and sessions on Welfare Rights (contributed by Parkhead Citizens Advice Bureau – PCAB) to service users as part of their ‘Other Activity’ hours included in their Community Sentence – Other Activity is used to address some of the underlying drivers of offending behaviour.
These sessions have been well received by the participants who were undertaking Other Activity as part of their Community Payback Order, with feedback on the mental health sessions being particularly positive (see charts 1-3 below).
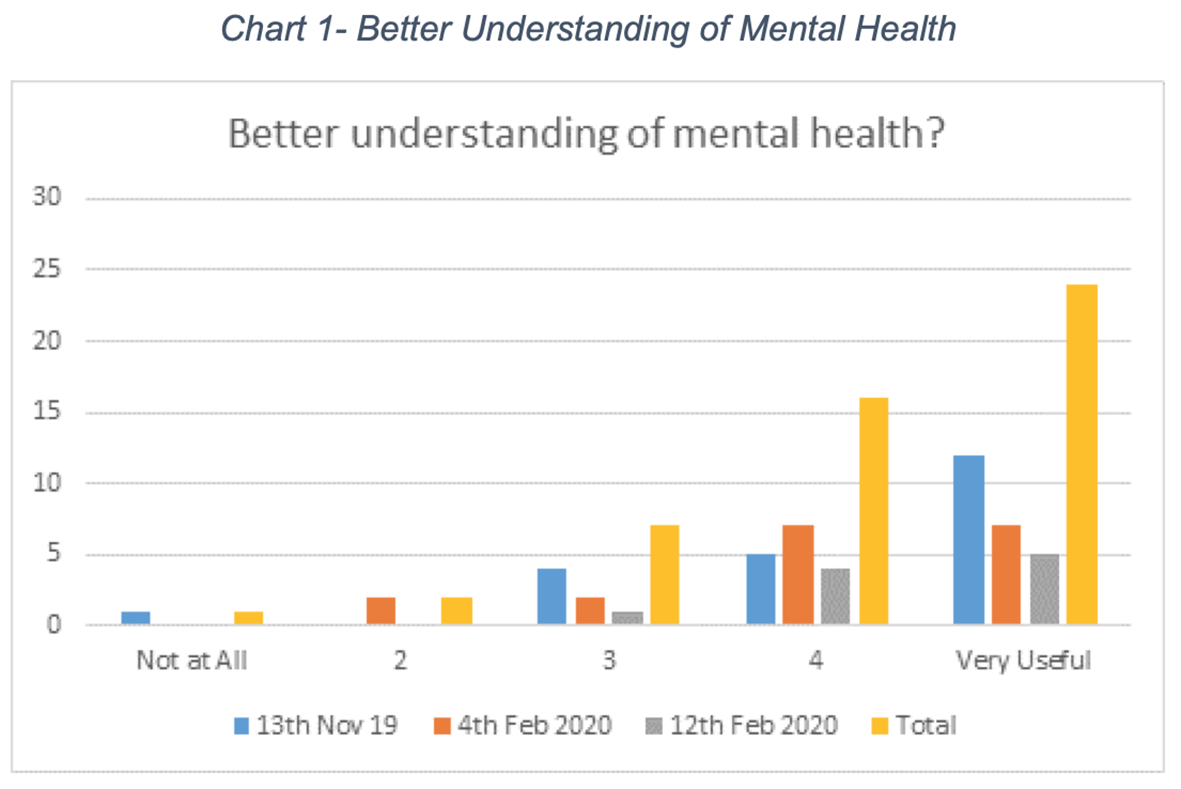
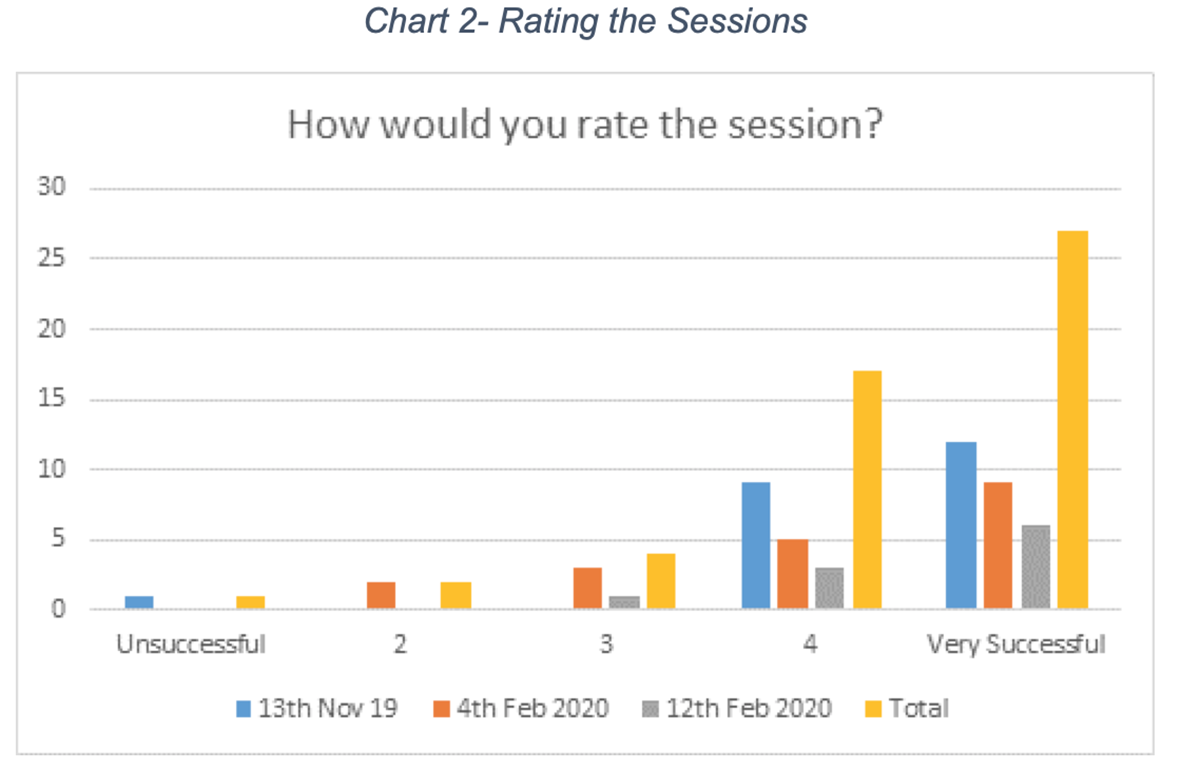
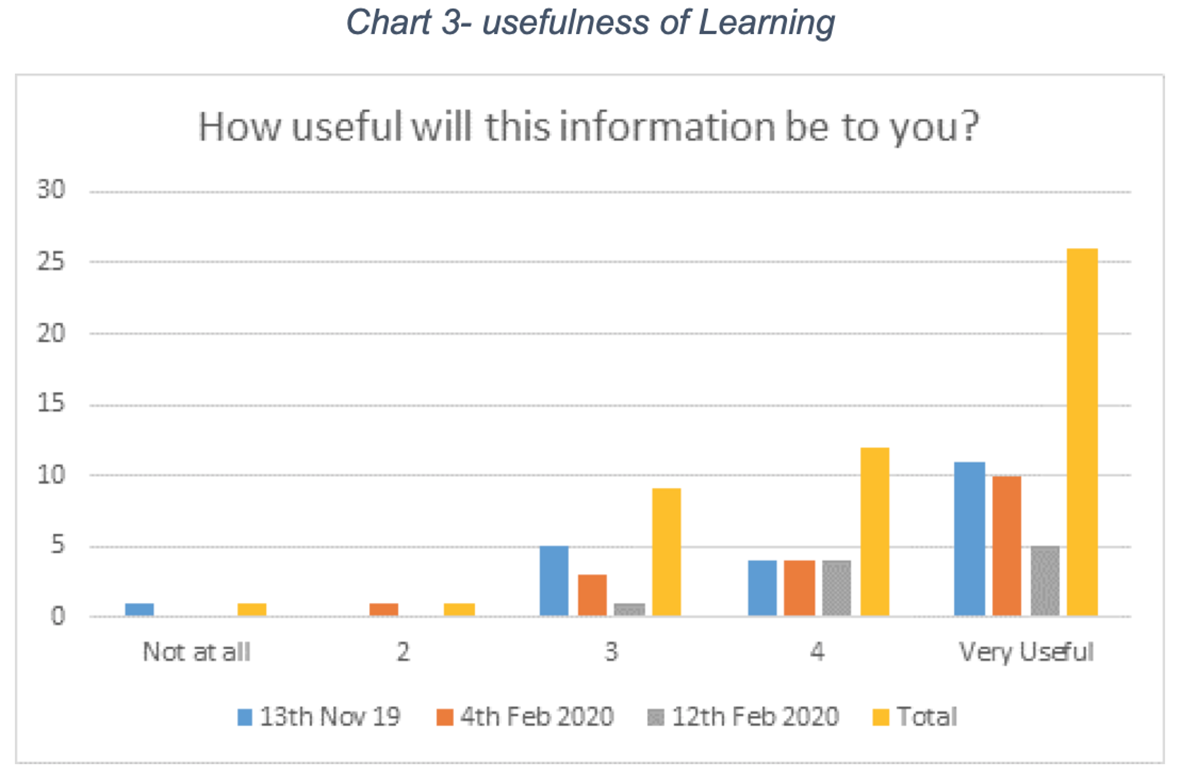
What participants said about the sessions:
“Learned a few things I didn’t know.”
“Nice people to speak to, made us feel comfortable”
“Gained a better understanding of helping family to cope with mental health”
“Never knew about that I could get a double appointment at doctors”
“Liked understanding of things never knew about”
“[I liked] their ability to talk so freely about mental health”
Further sessions on a wider variety of Service User identified themes are being explored to take forward over 2020/21.
Trauma Informed Practice Development and Training – To be trauma informed means to use understanding of the role that “violence and victimisation” play in the lives of individuals accessing services to “design service systems that accommodate the vulnerabilities of trauma survivors and allow services to be delivered in a way that will facilitate consumer participation in treatment” (Fallot, 2009). Importantly, ensuring that service delivery is trauma-informed does not require disclosure or treatment of trauma (British Columbia Centre of Excellence for Women’s Health, 2009).
Broadly, according to NHS Education Scotland, Trauma Informed Practice needs to include:
- Realising that traumatic experiences and their impact are an important consideration.
- Recognising the impact of trauma on service users.
- Responding to the impact of trauma by adapting their practice to be cognisant of trauma related difficulties (note that this doesn’t include treating the trauma).
- Resisting retraumatisation through focusing on safety, choice, empowerment, collaboration and trust (NHS Education for Scotland, 2017).
In similarity to the National Mental Health Improvement & Suicide Prevention Framework (NHS Education for Scotland, 2019), within the Transforming Psychological Trauma Framework (NHS Education for Scotland, 2017), NHS Education for Scotland identify four levels of practitioner competency when it comes to working with people with psychological trauma experience:
- Level 1 – Trauma Informed Practice;
- Level 2 – Trauma Skilled practice;
- Level 3 – Trauma Enhanced practice; and
- Level 4 – Trauma Specialist practice.
Level 1, Trauma Informed Practice is the NHS Education for Scotland, and by extension, the Scottish Governments expected minimum level of competency for all members of the Scottish Workforce.
As Glasgow is one of the national Trauma Training Pilot sites for Level 1 & 2 training, we have been working alongside partners, including the Anchor (NHSGG&C Psychological Trauma Service), to develop and plan delivery of this pilot. Unfortunately due to CoVid, those plans have been interrupted but we are now adapting for online and remote delivery formats. These will soon be available as an alternative to the face-to-face delivery previously offered and will be open to staff in NHS/HSCPs & other Justice Partners.
Additionally, we are exploring Training for Trainers developments that would enable organisations, agencies and services quality assured training packages to cascade to staff.
We are also working with an NHS Education for Scotland (NES) Funded NHSGG&C Training Coordinator Post (Level 3&4 Training) to support colleagues in Criminal Justice Services to identify their training requirements, and where required access the level 3 training pathway.
Crown Office & Procurator Fiscal Service (COPFS) Mental Health training – Mental Health and Well-Being was identified as a national priority across Crown Office & Procurator Fiscal Services (COPFS) in 2019. In January 2019, following discussion between the lead proposers of this project, a plan was agreed for delivery of training on Mental Health Awareness as relevant to the development of staff knowledge and understanding of the National Initial Case Processing Unit Procurator Fiscal (PF). The training session was delivered within 1hr at dedicated development time for staff, across three sites; Paisley, Falkirk, and Hamilton.
Staff responses to a pre-training questionnaire informed the development of the training within the context of Public Mental Health Improvement as it may assist the work of the National Initial Case Processing Team.
Training Aim: To increase knowledge and awareness of Mental Health, and the supports and services
Learning Objectives: By the end of the learning session participants will be able to:
- Understand the NHS Scotland definitions of Mental Health.
- Understand prevalence of mental ill health and mental distress in Scotland.
- Understand the interconnection between mental health and inequalities.
- Have an awareness of Mental Health Service Structures in Scotland.
- Have an awareness of common mental health problems and sources of support/relevant services.
- Have an awareness of self-care and resources that are available to support their own mental health and the mental health of those they care for.
Post-delivery feedback indicates an overall benefit from training delivery. The post-training questionnaire results, despite being small in number, accurately reflected the engaged discussion with staff and verbal feedback received by the trainers across the three sessions delivered (see Chart 4).
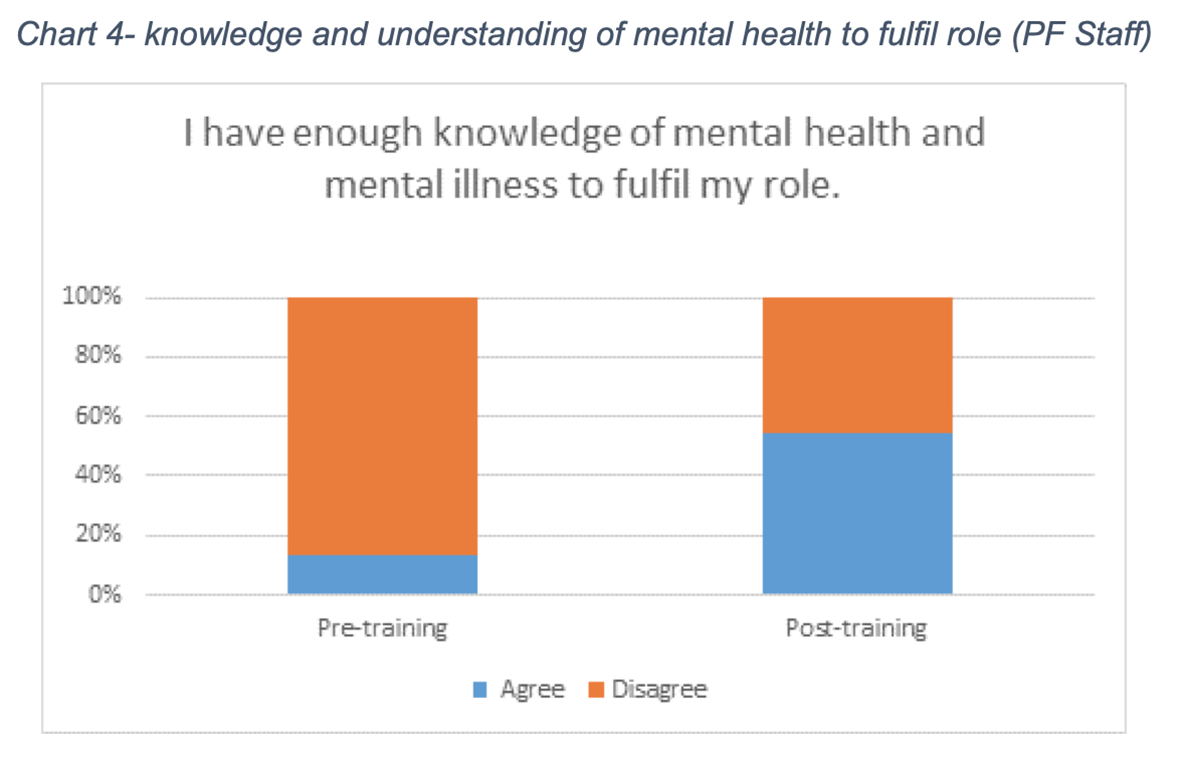
What some of the participants said:
“Much of the discussion made me stop and think and consider the stigmas and the gender based division”
“As discussed at the training there is frustration that the way each area deals with those in custody presenting with mental health/illness issues is different.”
The results of the questionnaire indicate a need for further training on specific aspects of mental health which requires exploration and raises a challenging perspective for the NHS regarding the provision of mental health services and assessments to services users of court and justice services.
A full report is available on NHSGG&C Stor Repository at: https://www.stor.scot.nhs.uk/handle/11289/580266.
Families Impacted by the Justice system – The report ‘Constructive Connections: building resilience of families affected by the criminal justice system’, A research project for NHS Greater Glasgow and Clyde, into the health and social impacts of the justice system on children and their families is now available for download at the Families Outside website and on the NHSGG&C Stor Repository.
Responses to the research are ongoing, aiming to improve the experience of children, young people and their families when they are impacted by the justice system.
We are working with Families Outside to develop a training package that incorporates the research findings from Constructive Connections and responds to the young people’s desire for adults to open conversations about their experiences of parental or familial imprisonment.
Families Outside have implemented a training pilot for multidisciplinary and multiagency staff working with children and young people. The training aims to disseminate the research findings in an accessible way, and in response to Children’s request for opportunities to talk about their experiences and find support, it also aims to encourage workers to open conversations with children and young people on imprisonment of family or important people in their lives.
Evaluation of the pilot training is in process, having been delayed by necessary service responses to CoVid and will be available later in the year, along with roll-out of practitioner training. I will report on this next year – WATCH THIS SPACE!
Building on the overwhelmingly positive response to the Children Harmed by Alcohol Toolkit (CHAT) Training offered in 2016/17, further CHAT training was commissioned from Alcohol Focus Scotland and delivered in 2019/2020. In addition, CHAT+ training (aimed at workers supporting children and young people who are looked after) was also commissioned as part of this programme of training.
Evaluation of the training is delayed by necessary service responses to CoVid. Anecdotal feedback reports a positive response to training and the resource usefulness for practice. Full evaluation report will be available later in the year with a 6month impact assessment of usefulness of the resource to participants practice. Again I will report on this next year – WATCH THIS SPACE!
As I said at the beginning of this article, the picture is complex, but I do hope that the initiatives laid out give you a flavour and better understanding of how Health can contribute to and deliver as part of the overall reducing re-offending agenda.